Whiplash Physio
Whiplash Physio Gold Coast | Robina Physio
By Jonathan Dorfzaun, Physiotherapist.
If you’ve been involved in a car accident and are now experiencing neck pain, headaches, stiffness, or dizziness, you may be dealing with a whiplash injury and likely will require Whiplash Physio.
At Robina Physio on the Gold Coast, we regularly assess and treat whiplash, neck pain, and associated headaches and dizziness—including cases that have not improved with rest, medication, or time.
Whiplash can be more complex than it first appears. However, with the right physiotherapy approach, most people can recover well and return to normal activity.
What Is Whiplash?
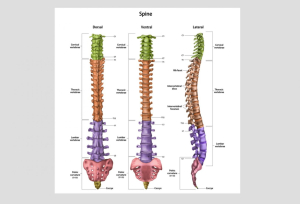
Whiplash is a rapid acceleration–deceleration injury of the cervical spine, most commonly occurring in rear-end motor vehicle accidents.
During impact, the neck undergoes a rapid sequence of:
- Extension (backward movement)
- Followed by flexion (forward movement)
This creates significant mechanical stress across multiple structures of the cervical spine.
Whiplash can affect:
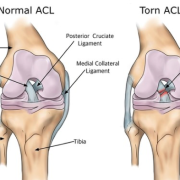
- Cervical facet joints (zygapophyseal joints)
- Intervertebral discs
- Ligaments, particularly the anterior longitudinal ligament and capsular ligaments
- Deep and superficial cervical muscles
- Neural structures, including nerve roots and the spinal cord
- Sensorimotor control systems, including proprioception and balance
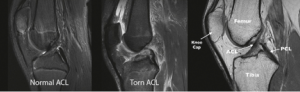
Importantly, many people with whiplash will have normal X-rays or MRI scans, yet still experience significant pain and dysfunction. This is because most whiplash injuries involve soft tissue, neuromuscular, and sensorimotor impairments, which are not well visualised on imaging.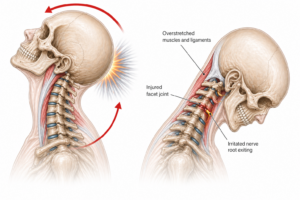
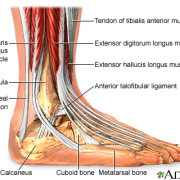
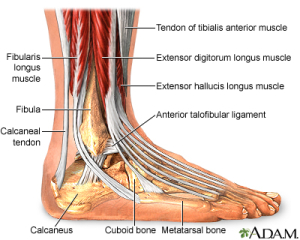
The Anatomy of Whiplash Injuries
To understand why whiplash symptoms can be persistent, it’s important to understand the anatomy involved.
Cervical Facet Joints
The facet joints are small joints at the back of the spine that guide movement. Research shows they are one of the most common pain generators in whiplash due to capsular strain during rapid extension.
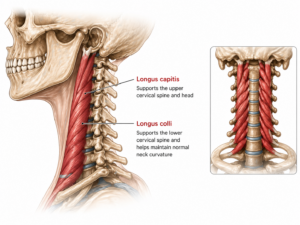
Deep Neck Muscles
The deep cervical flexors (longus colli and longus capitis) play a key role in:
- Segmental stability
- Postural control
- Fine motor control of the neck
Following whiplash, these muscles often show:
- Reduced activation
- Delayed timing
- Fatty infiltration in chronic cases
At the same time, superficial muscles like the sternocleidomastoid (SCM) and upper trapezius tend to become overactive, contributing to stiffness and pain.
Ligaments and Passive Stability
Ligaments such as the alar ligaments and transverse ligament provide passive stability to the upper cervical spine. While severe injury is rare, even mild strain can alter proprioceptive input, affecting balance and head control.
Nervous System Sensitivity
Whiplash is not purely a structural injury. It often involves:
- Peripheral sensitisation (increased sensitivity of injured tissues)
- Central sensitisation (increased responsiveness of the nervous system)
This can explain why pain persists long after tissues have healed.
Common Whiplash Symptoms
Whiplash symptoms may develop immediately or over the following 24–72 hours.
Common presentations include:
- Neck pain and stiffness
- Headaches (often originating from the upper cervical spine)
- Shoulder and upper back pain
- Reduced neck movement
- Pins and needles or numbness
- Dizziness or balance issues
- Jaw tightness or TMJ discomfort
- Fatigue and reduced concentration
These symptoms are commonly classified as Whiplash-Associated Disorder (WAD), ranging from mild to more persistent presentations.
👉 Many people we see for neck-related headaches physiotherapy are actually dealing with underlying cervical dysfunction following whiplash.
Why Do Whiplash Symptoms Persist?
A key reason people don’t recover is misunderstanding the injury.
Persistent symptoms are rarely due to a single damaged structure. Instead, they typically involve a combination of:
- Deep Muscle Dysfunction
Reduced activation and endurance of the deep cervical flexors leads to:
- Poor segmental control
- Increased strain on passive structures
- Overuse of superficial muscles
- Altered Movement Patterns
After injury, the brain may adopt protective strategies such as:
- Stiffening the neck
- Avoiding certain movements
- Over-recruiting large muscle groups
While protective initially, these patterns can become maladaptive over time.
- Sensorimotor Impairment
The neck has a high density of proprioceptors, which provide information about head position and movement.
Whiplash can disrupt this system, leading to:
- Dizziness
- Poor balance
- Difficulty with head-eye coordination
- Nervous System Sensitisation
The nervous system may become more sensitive following injury, resulting in:
- Heightened pain responses
- Increased muscle tension
- Ongoing symptoms without structural damage
This is why rest alone is not an effective treatment strategy.
Whiplash, Headaches and Dizziness: Why They Are Linked
Whiplash rarely occurs in isolation.
The cervical spine has strong connections with:
- Headache pathways (via the trigeminocervical nucleus)
- Vestibular system (balance and spatial orientation)
- Visual system (eye-head coordination)
- Jaw and TMJ function
This explains why many people experience:
- Headaches (cervicogenic headaches)
- Dizziness or “off-balance” sensations
- Jaw tightness or clicking (TMJ disorder)
👉 Effective treatment must address all of these systems—not just the neck.
What Does the Evidence Say About Whiplash Physio?
Modern research strongly supports an active, exercise-based approach to whiplash rehabilitation.
Key findings include:
👉 Active physiotherapy leads to better outcomes than passive rest
👉 Early movement reduces the risk of chronic pain
👉 Education improves recovery and reduces fear-avoidance behaviours
Effective treatment includes:
- Early, guided movement
- Strength and motor control retraining
- Gradual return to activity
- Education around pain and recovery
Outdated approaches such as prolonged rest, cervical collars, or complete activity avoidance are no longer recommended in most cases.
Whiplash Physio Robina: Our Approach
At Robina Physiotherapy, we take a structured, evidence-based approach to whiplash treatment.
Comprehensive Assessment
Your assessment includes:
- Cervical joint mobility and segmental assessment
- Deep neck flexor strength and endurance testing
- Movement pattern and motor control analysis
- Postural assessment
- Neural screening (including nerve mobility)
- Assessment of headaches, dizziness, and TMJ involvement
This allows us to identify the key drivers of your symptoms.
Targeted Treatment
Your treatment plan may include:
- Manual Therapy: Joint mobilisation to improve cervical movement and techniques targeting facet joint stiffness
- Soft Tissue Therapy: Release of overactive muscles such as SCM, upper trapezius, and levator scapulae
- Dry Needling: To reduce muscle tension and improve neuromuscular function
- Deep Neck Muscle Retraining: Specific exercises targeting longus colli and longus capitis. Progressive endurance and control training
- Sensorimotor and Vestibular Rehabilitation: Balance retraining. Head-eye coordination exercises
- Movement Retraining: Restoring normal, confident movement patterns
- Graduated Return to Activity: Including driving, work, gym and sport
Do You Need Physio If Your Scan Is Normal?
👉 Yes.
Imaging such as X-ray or MRI does not assess:
- Muscle function
- Movement control
- Sensorimotor integration
- Nervous system sensitivity
These are often the primary contributors to ongoing symptoms.
Physiotherapy focuses on restoring these systems, which is why it is so effective—even when scans appear normal.
Why Our Approach to Whiplash Is Different
At Robina Physio on the Gold Coast, we don’t just treat symptoms—we assess the underlying drivers of your pain.
This includes:
- Deep cervical muscle dysfunction (longus colli & capitis)
- Cervical joint irritation (facet joints)
- Sensorimotor and proprioceptive impairment
- Nervous system sensitisation
This level of assessment allows us to target the exact cause of your symptoms, rather than applying generic treatment.
When Should You See a Whiplash Physio?
You should seek physiotherapy if:
- Symptoms persist beyond a few days
- Neck movement is restricted
- Headaches or dizziness are present
- Pain is not improving
- You feel hesitant or fearful of moving your neck
👉 Early treatment is associated with faster recovery and reduced long-term symptoms
Whiplash Physio Gold Coast (Robina)
The physiotherapists at Robina Physiotherapy have extensive experience managing:
- Acute car accident injuries
- Persistent and chronic whiplash
- Neck-related headaches
- Dizziness and balance issues
- TMJ-related conditions
We take an evidence-based approach focused on:
- Reducing pain
- Restoring movement
- Improving strength and control
- Returning you to normal activity
Whiplash Physio – FAQs
How long does whiplash take to recover?
Most people improve within a few weeks. However, recovery time varies depending on injury severity, nervous system involvement, and how early treatment begins.
Can physio help chronic whiplash?
Yes. Even long-standing symptoms can improve with targeted rehabilitation addressing strength, movement, and nervous system sensitivity.
Should I rest my neck after whiplash?
Short-term rest may help initially, but early movement and guided rehabilitation are essential for recovery.
Do I need a referral?
No referral is required to see a physiotherapist. We regularly treat patients from across the Gold Coast including Robina, Varsity Lakes, Burleigh, Mudgeeraba and surrounding suburbs.
At Robina Physio on the Gold Coast, we specialise in providing accurate diagnosis and personalised treatment plans for whiplash and its associated complaints. Our experienced physiotherapists will assess your condition thoroughly, relieve your acute symptoms, and recommend effective, tailored exercises for ongoing relief.
Book Your Physio Appointment Online Now at Robina Physiotherapy